Key Takeaways
-
Laser hair removal offers a long-term solution for unwanted body hair, but costs can vary widely based on several factors, including the treatment area size, geographic location, and the provider’s expertise.
-
Understanding the factors that influence the cost of laser hair removal, such as the number of sessions needed and the type of laser technology used, can help you budget more effectively for your treatment.
-
The average cost breakdown shows that while initial sessions may seem expensive, laser hair removal can be cost-effective in the long run compared to traditional hair removal methods.
-
To save on treatment costs, consider package deals or special promotions offered by clinics, and don’t hesitate to ask about payment plans or financing options.
-
Choosing the right provider is crucial not only for ensuring effective results but also for your safety. Look for licensed professionals with good reviews and a track record of success in laser treatments.
-
Remember, the value of laser hair removal goes beyond just the cost. The convenience, confidence, and long-term savings on traditional hair removal products and services can significantly enhance your quality of life.
Understanding Laser Hair Removal
Process Explained
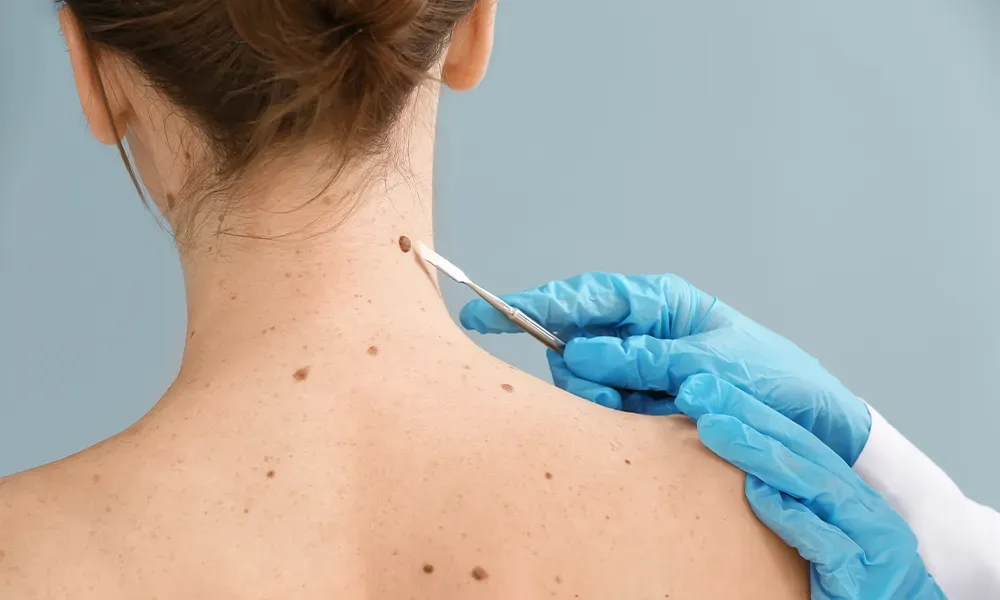
Laser hair removal uses concentrated light to target hair follicles. This light is absorbed by the pigment in the follicles, damaging them. It significantly reduces future hair growth.
The treatment is precise, targeting only unwanted hairs. It leaves surrounding skin undamaged. Multiple sessions ensure comprehensive coverage and effectiveness.
Benefits Highlighted
One major benefit is long-term hair reduction. Unlike shaving or waxing, laser treatments offer a more permanent solution.
It’s also highly precise, making it ideal for removing hair from sensitive areas. Patients appreciate the speed of each session, with large areas treated quickly.
Misconceptions Addressed
Many believe laser hair removal is extremely painful. However, advancements have made it more comfortable than often expected.
Another misconception is its ineffectiveness on certain hair types. While results vary, modern lasers work on a wider range of hair colors and skin tones than before.
Factors Influencing Cost
Treatment Area
The size of the treatment area plays a crucial role in determining the cost of full body laser hair removal. Larger areas, such as legs or back, require more time and resources, leading to higher charges. Conversely, smaller regions like the upper lip or chin are less expensive to treat. This variation is because larger areas demand more laser pulses to achieve desired results, increasing both the session’s duration and the overall treatment expense.
Clients should consider this aspect when planning their budget for hair removal. It’s not just about removing unwanted hair; it’s about understanding how each part of the body contributes to the total cost.
Geographic Location
The geographical location significantly impacts the price of laser hair removal treatments. Costs can vary widely between different cities and regions due to factors like local market demand and the cost of living. For instance, clinics located in metropolitan areas often charge more than those in smaller towns due to higher operational costs.
This variance means that individuals might find more affordable options by researching providers outside their immediate area. However, they must also factor in potential travel expenses when considering this option.
Practitioner Expertise
The expertise and qualifications of the practitioner also influence laser hair removal prices. Highly skilled professionals with extensive experience typically charge more for their services. This is because they offer a higher level of precision, potentially reducing the number of sessions needed for complete hair removal.
Patients seeking these treatments should weigh the cost against the benefits of working with an experienced practitioner. Investing in quality care can lead to better outcomes and ultimately save money by minimizing the need for additional sessions.
Average Cost Breakdown
Session Costs
The average cost of a single laser hair removal session varies widely. It typically ranges from $50 to $300. This price fluctuates based on the body area being treated.
Smaller areas like the upper lip or chin may fall at the lower end of this spectrum. In contrast, larger areas such as the back or legs command higher prices due to more extensive work involved.
Area-Specific Prices
For those considering full-body hair removal, understanding how costs differ by area is crucial. Here’s a brief overview:
-
Underarms: Around $150 to $250 per session.
-
Bikini Area: Generally costs between $150 and $450.
-
Legs: Full leg treatments can range from $600 to $850.
-
Back: This is one of the pricier areas, with sessions costing up to $900.
These figures highlight that larger body areas not only require more time but also significantly increase overall treatment expenses.
Total Treatment Costs
It’s important to remember that these prices usually cover the entire treatment process. This includes necessary pre and post-care, which ensures optimal results and skin health.
Multiple sessions are often required for complete hair removal, pushing total costs higher. However, many find this investment worthwhile for the long-term benefits of smooth, hair-free skin.
Saving on Treatment
Package Deals
Clinics often offer package deals for multiple sessions. This option can significantly lower the cost per session. Patients should inquire about these bundles during their initial consultation.
By opting for a package, individuals can save up to 20% off the total price. It’s a practical approach for those committed to full body hair removal.
Multiple Quotes
It’s wise to get quotes from several clinics. Prices can vary widely based on location, technology used, and the clinic’s reputation.
e may also have special offers or discounts for new clients. Comparing these quotes helps in finding the most cost-effective solution without compromising on quality.
Off-Peak Discounts
Consider scheduling treatments during off-peak seasons. Clinics might offer discounts during slower periods to attract more clients.
This strategy not only benefits your wallet but may also offer more flexible scheduling options. It’s a win-win situation for both the clinic and the patient.
Choosing a Provider
Certification Importance
Selecting a provider with proper certifications is crucial. They ensure safety and effectiveness in hair removal treatments. Providers should have credentials from recognized medical boards or aesthetic associations.
Look for clinics that boast a good track record. This reflects their commitment to quality and client satisfaction.
Consultation Advice
Scheduling consultations is a wise move. It allows you to discuss the provider’s experience and the technology they use. Ask to see before-and-after photos of previous clients.
These meetings offer insights into what you can expect. They also help gauge the provider’s expertise in full body hair removal laser treatment.
Financial Options
Discuss payment plans or financing options during your consultation. Full body laser treatments often require multiple sessions, making them pricier than other methods.
e clinics offer packages or discounts for multiple sessions. This can be a cost-effective solution for complete hair removal needs.
Closing Thoughts
Deciphering the landscape of full body hair removal laser treatment costs can feel overwhelming, but you’re now equipped with the knowledge to navigate it confidently. Understanding the factors that influence cost, from treatment areas to provider expertise, empowers you to make informed decisions tailored to your needs and budget. Remember, investing in a reputable provider not only ensures safety but also maximizes the value you get from your investment.
Taking the plunge into laser hair removal is a significant step towards achieving long-lasting smoothness and convenience. By considering the average cost breakdown and exploring ways to save on treatment, you’ve laid the groundwork for a successful journey. Now’s the time to choose a provider who aligns with your expectations and budget. Don’t hesitate to reach out for consultations; start your journey towards a hassle-free, hair-free life today.
Frequently Asked Questions
What is laser hair removal?
Laser hair removal is a cosmetic procedure that uses lasers to target and destroy hair follicles, resulting in the reduction of hair growth.
How does the cost of full body laser hair removal vary?
The cost varies based on factors like location, provider expertise, and treatment area size. It’s important to consult with providers for accurate pricing.
What is the average cost for full body laser hair removal?
On average, full body laser hair removal can range from $2,500 to $3,000 per treatment session. However, prices can vary widely.
Can I save money on my laser hair removal treatment?
Yes, look for package deals or special promotions offered by clinics. Some providers also offer financing options to spread out the cost.
How do I choose the right provider for laser hair removal?
Choose a provider based on their qualifications, experience, and reviews. Ensure they use FDA-approved laser technology and offer consultations to discuss your needs.