Key Takeaways
-
J-Plasma uses cold plasma technology to tighten skin and enhance tissue quality through tiny incisions, making it less invasive than surgical lifts yet still needing realistic expectations about the subtle results.
-
Ideal candidates have mild to moderate skin laxity, great tissue quality, and realistic expectations. Patients with extreme loose skin may require excision.
-
Results develop over time with early swelling and visible tightening. The most noticeable improvements occur at about one month and final results appear around three to six months.
-
Pair J-Plasma with liposuction when applicable for superior sculpting. Adhere to post-care compression garments and activity limitations to facilitate recovery.
-
Compare J-plasma before and after pictures closely for uniform lighting, angle, and pose. Check a few samples across body areas to avoid being misled.
-
Know the risks like bruising, numbness, and rare complications. Select a skilled, certified surgeon. Maintain healthy lifestyle habits for long-term results.
J-plasma results honest before and after expectations describe typical outcomes and likely recovery after the procedure. This innovative treatment uses cold plasma to tighten the skin and reduce loose tissue with visible contour changes within weeks.
The most common short-term side effects are swelling and bruising, which abate within days to weeks. Long-term results vary based on skin quality, age, and surgeon technique.
The body is all real before-after photos, patient timelines, and realistic expectations.
The Technology
J-Plasma Renuvion mixes helium gas with radiofrequency energy to generate a targeted beam of cold plasma that enhances skin tightening and tissue quality. The device provides energy in a controlled fashion to the subdermal plane, briefly heating the tissue and inducing an immediate contracture as well as a longer-term collagen response.
This results in immediate tightening and remodeling over the course of months, with skin tone and firming, not bulking, removed.
How It Works
A small J-Plasma cannula is introduced subdermally through micro-punctures. The surgeon sweeps the cannula over the treatment area, and the device generates helium-plasma energy immediately above the tissue surface, controlling thermal spread and preserving surrounding structures.
Used alongside liposuction, J-Plasma addresses the skin post fat removal. Liposuction removes the fat layer so the plasma energy can directly affect the undersurface of the dermis. This combination tends to result in improved contour and less residual sag than liposuction alone.
The energy creates an internal heating that stimulates fibroblasts and induces neocollagenesis. Collagen fibers contract and new collagen deposits over weeks to months support ongoing skin contraction. The heating is quick and limited, which limits the chance of extensive thermal damage observed with previous-generation technologies.
The invasiveness of the procedure is low in comparison with abdominoplasty or large excisions. Incisions are tiny, recovery is often shorter, and many patients are back to light activity within days. There is swelling and bruising, but there is less major downtime and less need for drains.
The Ideal Candidate
Patients with mild to moderate skin laxity who desire enhanced skin elasticity and a more sculpted body contour see the best results.
-
Age typically below or around mid-60s with decent skin quality
-
Localized skin looseness after weight loss or pregnancy
-
Moderate laxity that is not significant enough for excisional surgery
-
Good overall health and non-smokers when possible
-
Realistic goals and willingness to follow post-op care
Candidates should anticipate subtle to moderate enhancement, not dramatic elimination of sagging skin. Despite very large skin folds, massive hernias or advanced excess, surgical excision will probably be the only option to obtain predictable results.
Treatment Areas
-
Abdomen
-
Arms (batwings)
-
Thighs (inner and outer)
-
Neck and jawline
-
Around the knees and bra roll
J-Plasma effectively treats both small focused zones and larger regions by varying pass technique and energy delivery. It can assist in firming abdominal skin, tightening arm skin, or reducing cellulite or stretch marks by firming the dermis.
|
Area |
Typical Improvement |
Notes |
|---|---|---|
|
Abdomen |
Moderate tightening |
Best with concurrent liposuction |
|
Arms |
Noticeable firming |
Good for mild batwing laxity |
|
Neck |
Subtle contouring |
Useful for early jowling |
Realistic Outcomes
J-Plasma can provide modest to significant skin tightening based on individual characteristics. It’s more a contour-refining option than a replacement for full-blown major excisional surgery. Before discussing recovery phases, remember that expectations need to be in line with skin quality, age, and the degree of laxity. Before-and-after photos give you a realistic expectation of probable transformation.
1. Immediate Effects
Anticipate swelling and bruising immediately post-treatment, commonly reaching a zenith during the initial 48 to 72 hours. Tightness is typical; the treated area may feel tight and pulled.
Most patients experience mild lifting and surface smoothing immediately. This initial enhancement is incomplete and can be obscured by postoperative edema. Some temporary numbness or strange sensation around the incision sites is normal and typically improves over a few weeks.
Watch for signs of problems: increasing severe pain, growing fluid pockets, or spreading redness. Report these early to the clinic for timely care.
2. Initial Healing
Usually, compression garments are prescribed to reduce swelling and assist tissue as it settles. Wear time varies but often lasts days or weeks. Fine massage, when recommended, can smooth out small lumpiness and enhance comfort in addition to your opioids or anti-inflammatories.
Bruising and soreness subside. A little discoloration may persist for a week or two. Maintain a basic log or initial pictures to monitor adjustments and observe how tightness moves in this period.
3. Developing Results
Skin retraction persists for weeks as collagen shrinks and remodels. This remodeling yields smoother contours and less surface laxity gradually instead of immediately.
A lot of patients experience a perceived difference as early as four weeks, to what extent varies. These realistic outcomes, evidenced by regular photos every 2 to 4 weeks, provide clear proof of progress and can help keep your expectations in check when changes are subtle.
4. Final Appearance
Final results typically float somewhere between three and six months post-procedure when swelling has subsided and collagen has fully matured. Results can be permanent as long as weight is maintained and skin quality is decent.
Some swelling or minor contour irregularities can continue beyond 6 months. Define your goals according to realistic change. J-Plasma smoothes and firms; it doesn’t get rid of excess skin in large quantities.
5. Influencing Factors
Age, baseline skin thickness, amount of fat removed and tissue quality all contribute greatly to outcomes. An experienced doctor and a methodical approach make a difference for balance and evenness.
Post-op care includes wearing compression diligently, steering clear of heavy gym work early, and adhering to wound care. These factors impact not only your healing but your final appearance. Genetics and subsequent weight gain or loss will shift long-term results, so persistent weight helps provide a persistent advantage.
Analyzing Photos
Photos are king in judging j-plasma results. Pictures can fool unless you interpret them with care. Below are sharp tips to test photos for truth, followed by concrete examples and a simple checklist to use when you glance through before and after sets.
Lighting and Angles
Another lighting can conceal fine lines or create the illusion of smoother skin. Soft, diffuse light minimizes texture and harsh side light emphasizes every wrinkle. Photographed in warm, even light in the “after” shot but under cool, flat light in the “before” shot will exaggerate enhancement.
Camera height and tilt matter too. Shooting from above can tighten jawlines and reduce the look of a double chin, while a lower angle can make the neck look fuller. Contrast photos taken from the same level and proximity. Look for inconsistent shadows along the jaw or torso.
A missing shadow where it existed before can be a tip-off to a shift in light, not skin. Check for highlights on the skin. If a sheen is present in just one shot, water or oiling may be changing texture. If possible, verify that both pictures used the same focal length and exposure settings by using EXIF data.
Posing Differences
Posture changes can cause big visual transitions. Standing tall with your chin up stretches skin tight, while slouching exposes loose skin. Flexing the neck, clenching abs, or pulling shoulders back can simulate the impact of a procedure.
Photos where the subject is turned a bit to the side in one and faces forward in the other are not fair comparisons. Standardized poses remove this variable: neutral face, relaxed neck, arms at sides, same foot placement. Request a series of photos containing the same poses and expressions.
Good ones associate a relaxed front, neutral side, and flexed only if both before and after have the same movement.
Realistic Timelines
Tissue contraction can be evident immediately. Short-term results may be observed within 1 to 2 weeks, whereas real remodeling requires 3 to 6 months or more. Anticipate swelling and bruising initially, some tightening in weeks, and continued improvement over months as collagen develops.
Here’s a quick timeline for reference.
|
Time after procedure |
Typical signs |
|---|---|
|
0–2 days |
Swelling, redness, bruising |
|
1–2 weeks |
Reduced swelling, early tightness visible |
|
4–12 weeks |
Noticeable skin remodeling begins |
|
3–6 months |
Maturation of results, clearer contour |
Observe aftercare. Delayed healing blurs results and resist judging full benefit before three months.
Checklist for Photo Review
-
Same lighting, camera, distance, and focal length
-
Identical pose and expression in both images
-
No dramatic changes in clothing or skin sheen
-
Multiple examples across ages, body types, and treated areas
-
EXIF or clinic notes when possible for verification
The Recovery Journey
Recovery after J‑Plasma is staged and predictable when you follow specific care steps. Immediate post‑op care involves rest and protection. The first month includes gradual activity and tissue settling. Long‑term maintenance consists of preserving contour and skin quality. Mark each stage with a straightforward checklist to identify progress and assistance requirements.
First Week
Rest and limited activity are key during these initial seven days to reduce the risk of bleeding or delayed healing. Sleep with your head elevated for face work or avoid bending and heavy lifting for body work. Wear compression garments as your surgeon directs; they suppress swelling and encourage the skin to reattach itself to underlying tissue.
Change dressings as directed and keep incisions clean and dry to avoid infection. Swelling and bruising typically reach their worst during this time frame then gradually subside. Numbness or tightness can be anticipated. Pain is usually mild to moderate and controlled with prescribed pain meds and low-setting cold packs.
Be alert for rising redness, fever or drainage—these are called the clinic signs. Keep a recovery diary: note pain levels, meds taken, garment hours, and any odd symptoms.
First Month
Activity may increase gradually over weeks two to four, progressing from light walks to normal daily activities while continuing to exclude exertion. Compression use continues but can taper; follow your surgeon’s timing. Swelling diminishes and skin starts to feel taut. Ultimate contour is not determined.
Once clear, a gentle massage can help soften fibrous spots and promote lymph flow. Use very light pressure and simple circular motions. Hydration and protein-rich foods assist repair. Strive for a consistent daily intake of water and balanced meals.
Plan a follow-up visit in about week four to check on early outcomes, inquire about scars, and modify any garment plans.
Long-Term Care
Weight maintenance is key to permanent J‑Plasma results. Significant weight gain or loss can alter the result. Daily, light exercise maintains muscle tone under the treated skin and promotes circulation. On the recovery journey, a diet rich in adequate protein and nutrients promotes long‑term tissue health.
Protect treated areas from sun to avoid pigmentation changes and use gentle skincare, including moisturizers, sunscreen with SPF 30 or higher, and, if recommended, collagen-supporting topical agents.
Schedule regular clinic check-ins at six months and annually to track outcomes and address any late complications. Save your recovery diary long term to capture subtle changes and to provide future doctors with records of improvement or lack thereof.
Potential Risks
J-Plasma employs cold plasma energy to firm skin and decrease laxity. It can provide visible shifts, but it introduces predictable hazards that are significant for preparation and rebound. Here’s a ground-level view of what can go wrong, how often, and what reduces those risks.
List possible side effects: bruising, swelling, numbness, and temporary discomfort.
Post-J-Plasma, the majority of patients experience bruising and swelling in the treated areas. Bruises can be light purple marks or deeper discoloration and typically resolve within one to three weeks. Swelling is typical for a few days and can linger for up to six weeks in some cases, particularly after larger regions are addressed.
Temporary numbness or abnormal sensation in the vicinity of incisions or treated skin is common. Nerves are inflamed by heat and handling and sensation generally comes back over several weeks to months. Mild to moderate pain is expected and frequently treated with over-the-counter pain medications or brief regimens of prescription drugs.
Cold packs, elevation, and compression garments hasten relief. Anticipate brief stints of limited activity as the swelling and pain diminish.
Warn about rare complications such as burns, infection, or uneven results.
Rare but serious problems are thermal burns, infection, and contour irregularities. Burns happen if settings are too high or if it’s misused, creating deeper skin trauma that could require wound treatment or revision. Infection is rare with sterile technique and appropriate aftercare, but when it does occur, it may necessitate oral or IV antibiotics and, in extreme cases, surgical drainage.

Uneven outcomes appear as asymmetry, rippling, or localized skin laxity. These may arise from irregular energy transmission, inadequate tissue contraction, or patient variables such as scar tissue. Revision or other modalities might be necessary to fix visible abnormalities.
Note that risks are minimized when performed by experienced, certified plastic surgeons.
Complication rates decrease substantially with trained clinicians and consistent J-Plasma experience. Board-certified plastic surgeons know anatomy, know how to set device parameters appropriately, and know how to guard nerves and vasculature.
They give explicit preop screening and postop plans. Request before and after shots, complication rates, and references. Accredited facilities, like hospital outpatient centers or licensed surgical suites, provide another margin of safety.
Advise awareness of individual risk factors based on medical history and treatment area.
Personal factors alter risk ratings. Smoking, diabetes, autoimmune disease, poor nutrition, blood thinners and previous surgery all increase the risk of delayed healing, infection and poor cosmesis.
Points of thin skin or scar tissue, such as the neck, hands, or lower eyelids, pose an increased risk of noticeable surface irregularities or prolonged anesthesia. Talk full medical history, medications, and realistic goals with your surgeon so they can customize the procedure or recommend alternatives.
The Patient Perspective
Patients turn to J‑Plasma to firm loose skin, recover faster than with surgery, or take a less aggressive approach before going all the way. Most select it for minimal to moderate laxity on the face, neck, arms, abdomen, or thighs when they desire enhancement with no lengthy incisions. Others want a mix: a surgical lift where needed plus J‑Plasma to refine edges and smooth irregularities.
Cost, a desire to avoid general anesthesia, and a quick return to work or travel are decision drivers.
Common reasons patients choose J‑Plasma
People pick J-Plasma for three main reasons: firmer skin, shorter downtime, and a non-surgical or hybrid path. Smoother, tighter skin results from heating tissue in a controlled manner to induce immediate tightening and collagen build-up over months.
Less downtime has a lot of people experiencing days to a few weeks of swelling and bruising, not weeks of bed rest. Non-surgical looks appealing to those afraid of big incisions or extended anesthesia, professionals who can’t take long time off, or seniors who want less strain on their bodies.
Testimonials on outcomes and confidence
Patient anecdotes typically mention contour improvements at a few weeks and more defined outcomes at three to six months. One talked about looser upper arm skin that appeared smoother and let her wear sleeveless clothes again.
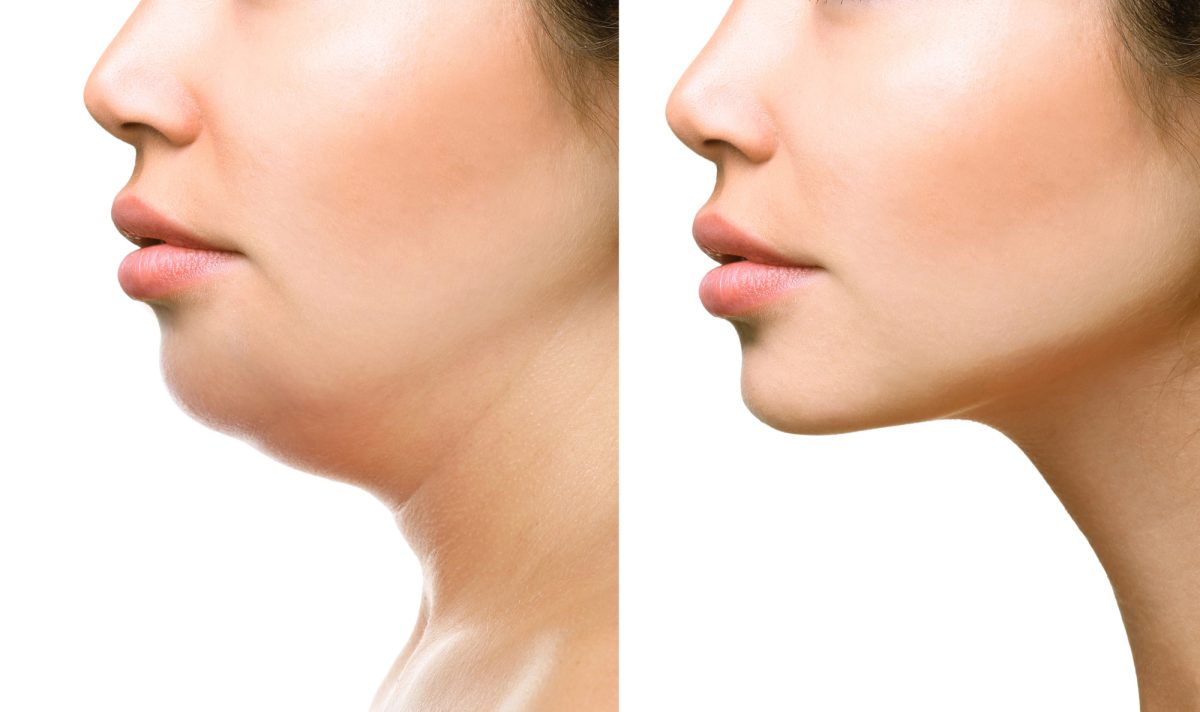
Another noted an improved jawline definition following neck treatment, which enhanced how clothes and makeup sat. Satisfaction connects to small, achievable improvements; the patient anticipating a full surgical lift is usually let down.
Several reference a confidence boost related to small changes consistently made as opposed to one dramatic change.
Concerns about pain, recovery, and expectations
Pain is usually mild to moderate and handled with short courses of oral painkillers. Some report more discomfort when treating thicker tissue areas. Recovery profiles vary.
Facial or neck cases often heal faster than abdominal or thigh work, where swelling can last longer. Scarring is minimal compared with open surgery, though small entry points exist.
Realistic expectations matter. J-Plasma can improve but not recreate youthful tissue where severe laxity exists. Providers should show before-and-after photos from similar cases and explain likely timelines.
Early tightening, progressive collagen gains, and final look occur at three to six months.
FAQs compiled from past patients
Useful FAQs include: How long does swelling last? Often 7 to 21 days depending on the area. Will I require additional treatments? Some require one touch-up at six months.
When can I work out? Light activity at one week and full exercise at four weeks typically. How much change is typical? Modest to moderate change is ideal for mild to moderate laxity.
Who is not a candidate? If you have very loose skin or an active infection, you should explore other alternatives.
Conclusion
J-Plasma tightens skin and smooths small wrinkles with minimal blood loss and brief downtime. Most patients observe gradual transformation over weeks and months, not immediate drastic transformations. Pictures establish definite targets. Recovery involves mild to moderate soreness and swelling for a few days, and most folks return to normal activities within about a week. Complications aren’t common, but they are real, and nerve or skin problems can happen. Chat one-on-one with a board-certified doctor, explore authentic before-and-after photos that match your age and skin type, and inquire about touch-ups and follow-up care. If you’re looking for firmer skin with minimal downtime, J-Plasma is worth consideration. Book a consult to receive a personalized plan and realistic expectations.
Frequently Asked Questions
What is J-Plasma and how does it work?
Here’s how J-Plasma uses cold plasma energy to heat and tighten skin. It treats superficial and deeper layers with limited thermal diffusion. Results come from immediate tightening and long-term collagen remodeling.
What realistic results can I expect after J-Plasma?
Anticipate skin tightening and a smoother skin texture. Results are different depending on your age, skin laxity, and area of treatment. Most experience improvement in weeks, with continued improvements over 3 to 6 months.
How should I evaluate before-and-after photos?
Watch for consistent lighting, angles, or expressions. Instead, want photos from board-certified providers and lots of cases. Request non-photoshopped pictures and patient schedules for reference.
How long is recovery and when do results appear?
Downtime is commonly 3 to 10 days of swelling and bruising. First tightening shows within days. Best results generally appear over 2 to 6 months as collagen regenerates.
What are the common risks and side effects?
Typical side effects are swelling, bruising, temporary numbness, and redness. Rare risks are infection, scarring, or uneven contour. Opt for a seasoned surgeon to minimize risk.
Who is a good candidate for J-Plasma?
Good candidates have mild-to-moderate skin laxity and reasonable expectations. It is perfect for those desiring skin tightening without the extensive surgery. A consultation will determine if it is a good fit.
How do I choose a qualified provider?
Select a board-certified plastic surgeon or dermatologist with J-Plasma experience. Check out before and after galleries, patient reviews, and inquire about how they handle complications and follow-up care.