Key Takeaways
-
Pannus, or apron belly, is excess skin and fat that can result from obesity, genetics, pregnancy, or weight fluctuations. It affects both physical health and self-esteem.
-
Removal options range from surgical panniculectomy and abdominoplasty to minimally invasive techniques and even non-surgical interventions like lifestyle changes.
-
Professional evaluation is important to determine the grade of pannus and to select a treatment plan tailored to individual health needs and cosmetic goals.
-
Post-operative care, a healthy lifestyle, and regular follow-ups are key for recovery and long-term success.
-
Psychological support and realistic expectation management assist patients in adapting to body image changes and enhance quality of life.
-
Consulting with qualified healthcare providers and understanding potential risks, costs, and benefits are essential steps before deciding on pannus removal.
Apron belly (pannus) removal options include surgery, lifestyle changes, and non-surgical treatments. Choices like panniculectomy or abdominoplasty work for those who want surgery.
For less invasive ways, some try exercise, healthy food, and special garments. Doctors may suggest different plans based on health, goals, and budget.
Each option comes with pros, risks, and costs. This guide walks through these options to help people find what fits best for them.
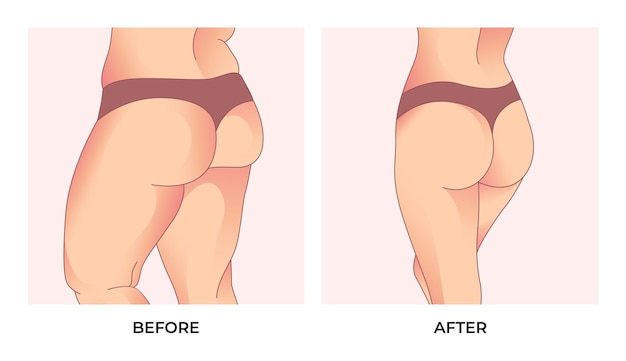
Understanding Pannus
Pannus is the term for the extra skin and fat that hangs down from the lower belly. This often happens after a person loses a lot of weight or has been living with obesity for a long time. Sometimes, it shows up after pregnancy or as people get older.
The skin can lose its stretch and this leads to the apron-like fold many know as an apron belly. Panniculectomy is a surgery that removes this extra tissue but does not tighten muscles, which is the main difference from a tummy tuck.
The Causes
Obesity is the biggest cause of pannus. As fat builds up in the belly, the skin stretches far past its limit. After weight loss, the skin doesn’t always snap back, leaving a hanging fold.
Genetics play a major role. Some people have genes that make their skin less stretchy or shape their bodies in a way that makes pannus more likely.
Pregnancy and childbirth are other typical contributors. As the belly expands quickly, the skin and muscles stretch to accommodate the baby. After delivery, the skin may not ‘snap back’, particularly after multiple pregnancies.
In addition to these, your age causes your skin to be less elastic, and sudden weight changes can cause skin to sag in difficult to repair ways.
The Grades
Doctors use a grading system to sort how severe a pannus is. Grade 1 is mild, where the skin just covers the pubic area. Grade 2 goes to the upper thigh, and Grade 3 falls to the mid-thigh.
Grades 4 and 5 are more severe, reaching the knees or even lower. A higher grade means more skin and fat, which can make movement tough and daily care harder.
Treatment options depend on the grade. Milder cases may be managed with lifestyle changes. Severe grades often need surgery, like a panniculectomy.
The choice of treatment is best made after a full check by a health expert, who can judge the extent and suggest the right plan.
The Impact
Pannus can cause real discomfort. Skin under the fold may get sore, red, or even infected. Moving can be hard, especially when walking or bending.
Sweating in the folds adds to skin problems. Some people experience back pain from the extra weight hanging off the belly, which throws off posture.
Living with pannus can hurt how people feel about themselves. Many feel embarrassed or worry about how others see them.
This can lead to less social activity or even avoiding relationships. The long-term health risks, like recurring skin infections, make it more than a cosmetic concern.
Panniculectomy Explained
A panniculectomy is surgery to take away extra skin and fat from the lower belly. This apron of skin, called a pannus, can form after large weight loss, aging, pregnancy, or other surgeries. The main goal is to help people who have a heavy, overhanging belly that gets in the way of moving, causes health troubles, or affects how they feel about themselves.
A panniculectomy can help with both health and looks, but it is not the same as a tummy tuck or liposuction. Tummy tucks tighten belly muscles and skin, while liposuction takes out fat but not loose skin. Knowing what a panniculectomy does—and does not do—helps people pick the right surgery for their needs.
Medical Necessity
Doctors see panniculectomy as needed when the pannus causes health problems. These can include rashes, skin infections, sores, or trouble walking and cleaning the area. Sometimes the apron is so large that it makes it hard to exercise or fit into clothes.
To determine if surgery is required for health, physicians look for recurrent infections, skin breakdown or other medical history. They might request photos, test results, and treatment history. Occasionally, a panniculectomy is the only way to halt these issues.
Insurance may pay for this surgery if it is medically needed. Each policy is different. Many require proof that the pannus has caused ongoing medical issues and that other treatments did not work. It is key to talk to a doctor or insurance representative before making plans.
A medical team can assist in determining whether this surgery is appropriate for you. They consider your health, your history, and what will benefit you most.
Cosmetic Goals
Panniculectomy can assist individuals in feeling confident about their appearance. For others, removing the apron of skin creates a smoother body contour and allows clothes to hang better. It can enhance confidence and comfort.
The focus here is body contouring, not addressing a medical concern. Some desire the double whammy of health reprieve and aesthetic enhancement. Others desire to be more comfortable in public or with their significant others.
Aesthetic and reconstructive goals differ. Reconstructive means repairing a medical issue. Cosmetic is appearance. What really matters is knowing which one matters to you.
Outcome may be nice, not ideal. There will be scars and the skin won’t be completely flat. Physicians may display before-and-after images to assist in establishing realistic expectations of what surgery can and cannot accomplish.
Tummy Tuck Comparison
|
Feature |
Panniculectomy |
Tummy Tuck (Abdominoplasty) |
|---|---|---|
|
Main Goal |
Remove hanging skin/fat |
Remove skin, tighten muscles |
|
Who It’s For |
Health, mobility issues |
Cosmetic improvement, loose skin |
|
Muscle Tightened |
No |
Yes |
|
Recovery Time |
4–6 weeks |
4–8 weeks |
|
Scarring |
Below belly, permanent |
Lower belly, may be longer |
|
Cost (USD) |
$8,000–$15,000 |
$9,000–$16,000 |
|
Insurance Cover |
Sometimes |
Rarely |
Panniculectomy is most useful for individuals with pain, sores, or infections from hanging skin. Tummy tucks are for the person who wants a firmer belly and muscle repair.
Both carry hazards such as bleeding, infection, or fluid accumulation. Complication rates can increase from 8 percent to over 50 percent. Recovery is slow for both; rest is needed and heavy lifting is off-limits for weeks.
Patients don compression garments and might require assistance with swelling, bruising, and tightness. Choosing the right surgery involves discussing your objectives, medical condition, and priorities with a physician.
Removal Options
Apron belly, or pannus, can affect comfort, health, and self-image. There are several ways to address it, ranging from surgery to lifestyle changes. Choosing the right method depends on individual needs, goals, and health status.
Professional guidance is key, and long-term results matter as much as short-term changes.
-
Surgical procedures (panniculectomy, abdominoplasty)
-
Minimally invasive methods (endoscopic techniques)
-
Conservative measures include weight reduction, lifestyle modification, and non-invasive devices.
-
Combined approaches for tailored results
Personalized attention is key. There’s no one size fits all. A pro consultation goes a long way toward making sure you match up the best possible option to your needs. Both short term gains and long term impacts warrant consideration.
1. Surgical Procedures
A panniculectomy eliminates excess skin and fat from the lower abdomen. It can relieve issues such as rashes, irritation, and recurrent infections. Panniculectomy differs from a tummy tuck (abdominoplasty).
A tummy tuck tightens muscles and sculpts the midsection, whereas panniculectomy simply removes the overhanging skin. Both procedures employ incisions across the lower abdomen, typically from hip to hip. Drains assist in clearing fluid for a week after surgery.
Surgery takes a few hours and typically involves a hospital stay of around two days. Most experience pain and swelling initially, with the swelling subsiding within three months. Strenuous work may be on hold for three to six weeks, and exercise might be on hold for up to three months.
Scars are inevitable and may take a couple of years to fade. Choosing a board-certified plastic surgeon minimizes risk and maximizes results.
2. Minimally Invasive
Some may choose less aggressive approaches, such as endoscopic surgery. These utilize smaller incisions and specialized instruments to excise excess skin. The primary advantages are reduced scarring, reduced recovery time, and reduced post-operative pain.
Not everyone is cut out for these. They might be most effective for individuals with minimal loose skin or fat. Results may be more subtle. Make sure to inquire about these options during your consultation.
3. Non-Surgical Methods
Obviously, lifestyle changes such as eating right and exercising can aid in abdominal belly shrinking naturally. Diets and support groups provide guidance and impetus for sustainable modifications.
Non-invasive treatments such as laser therapy or radiofrequency can tighten skin to some degree, but these won’t eliminate voluminous folds. They can be handy post-weight loss or as a means to maintain surgical results.
Long term, staying active and eating well are essential for maintaining results.
4. Combined Approaches
Hybrid techniques, which combine, say, surgery with non-invasive skin tightening, can offer a nicer equilibrium between aesthetics and wellness. A joint plan might assist with both utility and aesthetics and satisfy everyone’s preferences.
A custom plan is best crafted with your care team. Discuss openly with your surgeon what matters most to you.
The Patient Journey
Apron belly removal is an incremental journey. Stage by stage, it shapes the outcome and experience. This journey requires continuous dedication, dialogue, and self-compassion. Acknowledging what lies in front of them, both on the personal and practical level, helps patients prepare.
Initial Consultation
Your initial consultation with a surgeon defines the patient journey. A surgeon goes over medical history, checks the abdomen, and hears out each patient’s goals. This is when patients ought to discuss their goals, express apprehensions about scars or pain, and inquire about the potential complications.
The surgeon tells you what the surgery will and will not do, so no one expects immediate or flawless outcomes. Occasionally, a couple of pre-op tests will be required. This could be blood work or a heart and lung check.
Bringing a prepared list of questions can help ensure nothing important is left out during this first visit.
Pre-Operative Steps
Diet and medication changes can begin weeks prior to surgery. Surgeons might request patients to discontinue some medications, such as blood thinners, and to abstain from tobacco. Even small changes, like opting for lighter meals, can reduce your risk of complications during and after surgery.
I’m glad you had someone assist post-op. Having that ride home and just a little bit of help with household chores makes convalescence less stressful. Mental preparation is equally important.
Knowing that healing is a process and that hiccups are part of it can empower patients in their own journey rather than make them feel helpless and anxious.
Recovery Timeline
Immediately after surgery, everyone feels sore and fatigued. Pain tends to decline significantly in the first week, with OTC pain medicine generally sufficient by the second week. Swelling is to be expected and patients wear compression garments for four to eight weeks to assist their body in acclimating.
Within a couple of weeks, most begin to walk short distances, but full exercise commonly must be postponed for two or three months. Others experience mild aches and pains for a few days. Your incision heals mostly in the first three months, but the scar can continue improving up to a year.
Resuming activities is gradual, with additional restrictions and boundaries. Final outcomes may not manifest until months later.
Long-Term Care
-
Maintain a balanced diet with enough protein and fiber
-
Stay active with low-impact exercise once healed
-
Keep skin clean and dry to avoid irritation
-
Wear loose-fitting clothes
-
Avoid smoking, which slows healing
-
Be on the lookout for swelling, pain, redness, or discharge at the incision.
They are the best way to catch problems early and monitor your progress. Patients need to be vigilant for symptoms of infection or abnormal pain and to seek assistance if something is amiss.
By sticking with care and taking each step, you help guarantee better, longer-lasting results.
Beyond The Scalpel
Panniculectomy and other apron belly removal surgeries do more than alter your body’s appearance. They are a journey of self-image, recovery, and support. These surgeries can impact more than skin and tissue; they can impact your confidence, routine, and mental well-being.
Psychological Shift
Many people with a pannus stomach have lived with discomfort and limits for years. The excess skin can hang over the thighs or genitals, making walking, standing, and sitting hard. Removing it often brings relief and a boost in confidence, but some patients still struggle with their new body image, especially if scars remain or if changes are not as dramatic as they hoped.
For others, surgery provides tangible improvements and a greater range of motion, allowing them to feel less weighed-down. Quality of life tends to be better. The mind can be tender in convalescence, particularly if hopes were raised. A counselor or therapist can help fill in any lingering body image issues.

Some patients find it beneficial to speak with others who have had similar experiences. Surgeons and care teams emphasize open discussion regarding mental health. Post-surgical patients who are experiencing feelings of depression or anxiety should explore accessing support. This can smooth out the emotional roller coaster of recovery.
Expectation vs. Reality
Others believe that a panniculectomy or tummy tuck will solve all their worries or provide quick, permanent weight reduction. The typical patient can expect to gain 4% of their body weight over 12 years. These are not weight-loss surgeries; they deal with skin and tissue.
Complication rates vary from approximately 8% to more than 50%. Edema and pain are expected for weeks, and wounds may require up to three months to heal. Although these scars are tiny—2 to 3 millimeters with liposuction—they can still impact body image.
A realistic outlook is key. Pre-surgery consultations help define expectations and clarify risks and benefits. When you focus on being more mobile and feeling stronger and healthier instead of just looking better, you’ll be more satisfied.
Lifestyle Integration
-
Maintain a nutritious schedule. It is amazing what balanced meals, daily walks, and gentle stretching can do to keep results in place and help your healing.
Post-surgery, a compression garment for a few weeks curtails swelling and sculpts the new physique. By beginning light exercise as soon as you’re cleared by your doctor, you help your body make the adjustment and keep the weight stable.
When you have support from a friend or loved one, these changes come much more organically. Joining a local or online support group provides a sense of community. Members often exchange healing, diet, and setback tips. This makes it easier to stay on track and build lasting habits.
Risks and Realities
Apron belly, or pannus, impacts daily life, limits movement, and raises risks for a range of health issues, from skin infections to heart disease. Considering removal surgery such as panniculectomy means facing not just the benefits, but medical and financial realities. Weighing these risks is key before making any decisions.
Knowing all the potential risks going into surgery is important. Panniculectomy complications can be mild to severe. Some results, such as scars or numbness, linger. Informed consent is more than a signature—it’s having transparent, candid conversations with your surgeon. Inquire about your own risk, particularly if you deal with diabetes, hypertension, or a history of healing issues. Weigh the relief the surgery can provide against the risks.
|
Potential Risk |
Description |
|---|---|
|
Infection |
Open wounds can get infected, especially if hygiene is hard to keep. |
|
Scarring |
Scars from surgery may be large and take years to fade. |
|
Delayed Healing |
Healing may be slow, especially in people with chronic illness. |
|
Numbness/Bruising |
These are common and can last for weeks after surgery. |
|
Blood Clots |
Surgery raises the chance of blood clots in the legs or lungs. |
|
Seroma/Hematoma |
Fluid or blood may build up under the skin post-surgery. |
Potential Complications
Things that can go wrong after surgery are wound infections, delayed wound healing, or seroma formation. Infection could present as redness, swelling, pain, or pus at the wound. Bruising and numbness are common in the first few weeks.
Watch for warning signs: fever, spreading redness, or sudden pain. Quick action can prevent little issues from becoming big. Adhering to all post-surgery steps, such as clearing the area, taking medicines, and going to checkups, can reduce your risk.
Question it if it feels wrong. Physicians rely on patients to complain of pain or changes.
Financial Considerations
Panniculectomy can run several thousand USD without counting missed time at work. Certain health plans will pay a portion of it if it is for medical and not cosmetic reasons.
Understand what your insurance will and will not cover before scheduling surgery. If insurance doesn’t aid, certain clinics provide payment plans or loans.
A healthier post-surgery immune system could translate to fewer skin or infection doctor visits, saving cash in the long run.
Choosing Your Surgeon
Select a surgeon who is well qualified medically and in terms of experience with panniculectomy. Seek board certification and review patient reviews.
Being comfortable with the surgeon matters. Effective communication allows you to establish clear objectives and feel secure in expressing concerns.
It is reasonable to see more than one surgeon. You can compare their responses and find out who hears the best.
Conclusion
Apron belly, or pannus, can weigh heavy on daily life. Many want a fix that feels right for them. Some go for surgery like panniculectomy, while others try steady weight loss, skin care, or support wear. Each choice brings its own needs and results. Doctors map out options, answer tough questions, and help set clear steps. Risks stand out, but real stories and small wins often show the way. No single path fits all. To move forward, reach out to a care team, ask for facts, and share your goals. Good info and honest talks help make strong choices that match your needs. Find support, stay open, and make the next move that feels right for you.
Frequently Asked Questions
What is an apron belly or pannus?
An apron belly, called a pannus, is extra skin and fat that hangs down from the lower abdomen. It often results from weight loss, pregnancy, or genetics.
What are the main options for apron belly removal?
Your primary choices are panniculectomy surgery, abdominoplasty or a traditional tummy tuck, and non-invasive approaches such as weight control and maintenance. Surgery is the only way to truly remove excess skin.
How does a panniculectomy differ from a tummy tuck?
A panniculectomy takes off just the hanging skin and fat of the lower abdomen. Tummy tucks tighten abdominal muscles and contour the waist.
Who is a good candidate for pannus removal surgery?
Good candidates are generally healthy, have stable weight, and experience discomfort or hygiene issues due to the pannus. A medical consultation is needed for assessment.
What are the risks of panniculectomy?
Risks include infection, bleeding, scarring, and delayed healing. There may be alterations in cutaneous sensation. Discuss risks with a qualified surgeon.
Is pannus removal covered by health insurance?
Insurance may cover panniculectomy if it is medically necessary, for example, due to skin infections or mobility issues. Cosmetic procedures are typically not covered.
How long is recovery after pannus removal surgery?
It typically takes 2 to 4 weeks to recover. Therefore, while the majority of individuals should be able to resume normal activities following this timeframe, complete healing may require additional time.