Key Takeaways
-
Retatrutide acts as a GLP-1 drug to promote weight loss and curb appetite. Its impact compounds when paired with nutritional modifications.
-
A protein, fiber, healthy fat, and complex carb-rich diet enables you to get the most health benefits out of retatrutide while maintaining optimal blood sugar and energy levels.
-
Adequate hydration and strategic meal timing may assist with hunger control, digestion, and optimize retatrutide’s metabolic effects.
-
Tackling common side effects like nausea and constipation head-on with smaller meals, high-fiber foods, and sufficient fluid intake can make everyone feel much better and be more likely to continue using the treatment.
-
As a complement to retatrutide, eating a nutritious diet of whole foods is a smart choice.
-
Lifestyle factors such as exercise, gut health, and mental wellness are important components when it comes to obtaining and sustaining results with retatrutide.
Retatrutide and diet what to eat primarily focuses on foods that assist in maintaining stable blood sugar levels and promote healthy weight fluctuations. Individuals frequently select meals rich in fiber, lean protein, and healthy fats while reducing consumption of foods with added sugar or few nutrients.
Fresh vegetables, whole grains, and lean proteins comprise the majority of meals. To assist in scheduling dishes and snacks, the following areas provide specific food lists and concepts to attempt.
Understanding Retatrutide
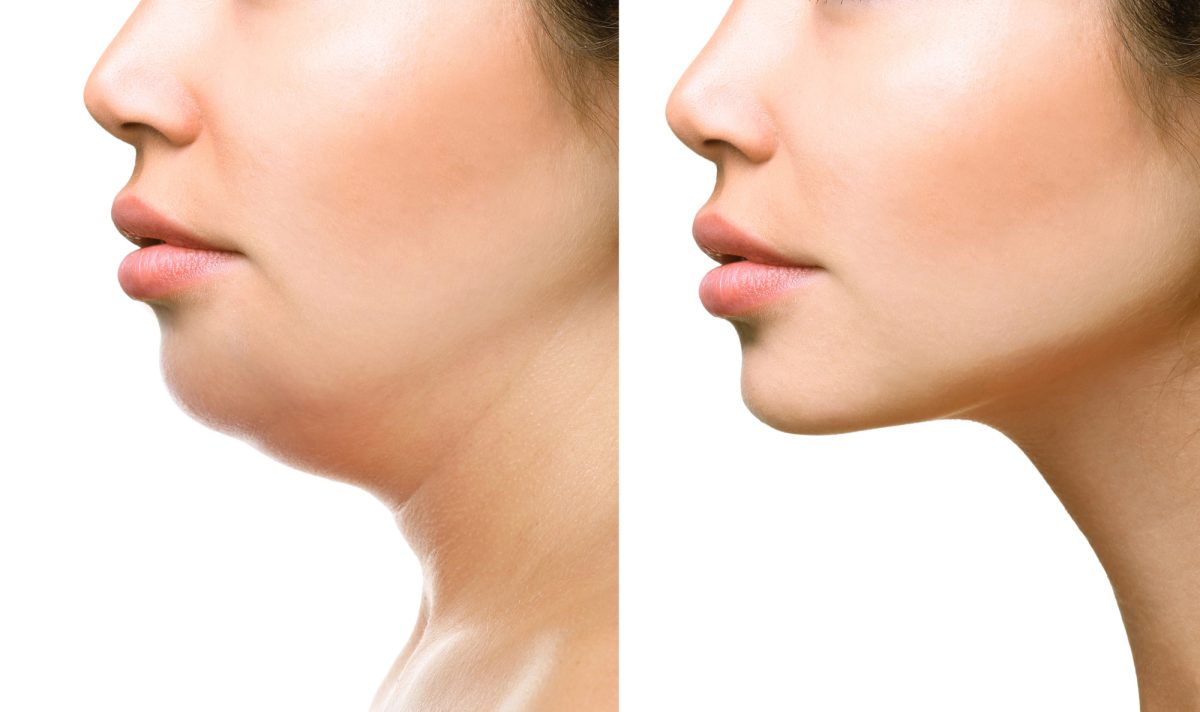
Retatrutide Overview Retatrutide is an experimental drug developed to treat obesity and type 2 diabetes. It stands out from other GLP-1 medications because it acts on three hormone pathways at once: GLP-1, GIP, and glucagon. This triple-pronged approach controls blood sugar, reduces appetite and may increase energy expenditure.
Retatrutide is administered once a week via injection, with doses generally initiated at a low level and increased gradually to mitigate side effects. Even in preliminary studies, retatrutide users can drop an impressive amount of weight — sometimes more than 20% of their initial body weight. This drug isn’t approved yet, but big trials are underway all around the globe. Pairing smart dieting with retatrutide may help patients experience more profound results and fewer side effects.
|
Feature |
Retatrutide |
Traditional GLP-1 Agonists |
|---|---|---|
|
Mechanism |
GLP-1, GIP, Glucagon |
GLP-1 only |
|
Dosing |
Weekly injection, titrated |
Weekly injection, titrated |
|
Effects on weight |
Average loss of 24–29% |
Average loss of 15–20% |
|
Appetite control |
Strong, multi-pathway |
Moderate |
|
Blood sugar control |
Enhanced, multi-pathway |
Good |
|
Clinical status |
Phase 3 trials |
Approved (various agents) |
The Triple-Action Effect
Retatrutide increases insulin secretion if blood glucose increases, facilitating the uptake of glucose from blood into cells. It delays gastric emptying, so blood sugar spikes less after a meal.
It’s on hunger centers in the brain, where it reduces cravings by silencing the signals that cause them, making it easier to commit to smaller meals. Individuals on retatrutide have described experiencing satiety more swiftly and maintaining that feeling longer than previously after meals.
Additionally, it resets the body’s energy burning. By targeting glucagon, retatrutide might increase energy expenditure and aid the body in accessing fat stores as fuel. This means more calories are burned at rest.
These changes accumulate. Blood sugar remains more stable, appetite is suppressed, and fat is more readily burned. The result is powerful weight loss and metabolic improvements beyond what the majority of single-action medicines can deliver.
Diet’s Role
A nutritious diet is key for anyone taking retatrutide, as the drug is most effective in combination with good habits. High fiber and protein foods aid satiety, while nutrient density supports overall health. You can reduce the risk of side effects like nausea by avoiding processed sugars and excess fats.
Some food groups to focus on include:
-
Whole grains (brown rice, oats, quinoa)
-
Lean proteins (fish, tofu, chicken)
-
Legumes (beans, lentils)
-
Vegetables of all types
-
Fresh fruits in moderate amounts
-
Healthy fats (olive oil, avocados, nuts)
Your diet can aid side effects. Having smaller meals that are frequent, keeping hydrated, and opting for blander foods when you first start the medication can help reduce stomach upset. Thoughtful nutrition assists your body through the transition, easing the treatment experience.
Core Nutrition Principles
Effective weight loss with retatrutide depends on smart nutrition decisions combined with sustainable lifestyle transformation. We want to lose fat, not muscle, while supporting metabolic health and making results stick. Balanced macros, nutrient density, individually tailored plans, and personalized strategies are far more important than any band-aid or trendy solution.
By staying goal oriented and striving for health instead of rapid weight loss, you’re less likely to get derailed. Type 2 diabetic individuals will make more gradual advances but still move in the right direction.
1. Prioritize Protein
Protein keeps muscle loss at bay and keeps you feeling satiated. It even revs your metabolism by forcing you to burn more calories digesting it than you burn digesting carbs or fat. Good sources include lean meats, tofu, lentils, eggs, and low-fat dairy.
For lunch and dinner, combine grilled chicken or fish with beans or quinoa, or indulge in a bowl of Greek yogurt and seeds. Protein can support steadier blood sugar and combat cravings. This is crucial with retatrutide, as the aim is fat loss, not muscle.
Try to incorporate a source of protein with each meal, even snacks.
2. Embrace Fiber
Fiber significantly contributes to digestive health and a sense of fullness. It delays digestion, which helps stabilize hunger and blood sugar. Whole grains, berries, carrots, broccoli, and oats are all simple ways to add fiber to your meals.
Both soluble and insoluble fiber count. Oats and apples contain soluble fiber, which cuts cholesterol. Insoluble fiber in whole wheat and veggies keeps things moving in the gut. Blend the two for optimal returns.
Fiber helps meals be more filling and encourages consistent weight loss over time.
3. Choose Smart Fats
Healthy fats keep your heart in shape and foster hormones. They’re best found in sources such as olive oil, nuts, seeds, and avocados. Omega-3 fats from fish or chia seeds combat inflammation and enhance metabolic health.
Fats pack calories, so portion them tightly. Drizzle a spoonful of olive oil on your salads or nibble on a handful of nuts. Healthy fats assist your body in utilizing vitamins A, D, E, and K, which are essential for health on any diet.
4. Mindful Carbohydrates
Choose complex carbs, such as brown rice, sweet potatoes, and legumes, in place of refined sugars. These offer lasting energy and help fuel daily movement. Carbs are essential for mind function. Timing and servings are key.
Combine carbs with protein and healthy fats to give you longer-lasting energy. This does a good job of preventing blood sugar from spiking. Portion control and surrounding carbs with periods of higher activity are important.
5. Hydration is Key
Water facilitates every bodily function, particularly when dropping pounds. Getting your 1.5 to 2 liters a day keeps your metabolism revving and can make you less hungry. Hydrating foods, such as cucumbers, watermelon, or oranges, contribute to your fluids.
Staying hydrated will help you control hunger and boost energy. This matters for anyone desiring sustainable weight loss with retatrutide.
Meal Timing Synergy
Meal timing modulates the body’s response to hunger, energy, and metabolism, particularly in conjunction with drugs such as retatrutide. Meal spacing at regular times can help the body acclimate to appetite changes that accompany treatment. When you eat moderate, balanced meals with protein, fiber, and healthy fats, you stay fuller for longer stretches. This dampens the craving to snack on sugary or fatty foods, which can make blood sugar swing and burden digestion.
Meal timing ties to energy utilization by the body. Eating pre and post exercise will assist muscle recovery and keep energy levels stable. For most, the post workout period is an ideal time to eat a nutritious meal with ‘good’ slow digesting carbs, protein, and fiber. This has the potential to help the body utilize nutrients effectively and could bolster the efficacy of treatment.
For example, a bowl of lentils with brown rice, steamed vegetables, and grilled tofu or chicken plays nicely together post-workout. On lighter days, meals and small snacks with fruit, nuts, or whole-grain crackers can keep your energy even without taxing the system.
Checklist for using meal timing to support results:
-
Eat within 1 to 2 hours of waking up: Jumpstarts metabolism and keeps energy from dipping.
-
Time meals around physical activity: A little snack with carbs and protein 30 to 60 minutes before movement can really fuel your performance. A balanced meal afterward aids muscle repair and recovery.
-
Spread meals and snacks throughout the day. Eating every 3 to 5 hours can prevent massive hunger fluctuations that cause you to overeat.
-
Avoid heavy, greasy, or sugary foods late at night. This supports better sleep and lets the gut rest.
-
Drink water with and between meals. This keeps hydration in check as some medications can blunt thirst cues.
-
Pay attention to hunger signals: While digestion can slow with some treatments, that doesn’t mean you should eat until you’re stuffed. Stop eating once you’re satisfied.
Meal spacing is good for fullness and cravings control. Missing those long spaces between meals usually means less opportunity to binge when you finally dig in. If appetite wanes in the evening, as it does for some on retatrutide, a light dinner or even a late-night snack can be skipped.
The idea is to align meals with natural hunger, not habit or clock.
Managing Side Effects
Retatrutide, similar to other GLP-1 and GIP receptor agonists, can induce side effects that frequently alter people’s eating habits and meal planning. Nausea, vomiting, diarrhea, and constipation are the most common, particularly when initiating or increasing a dose. Clinical trials found nausea to peak following dose escalations, particularly above 8 mg.
Other effects such as redness and itching at injection sites, increased resting heart rate, and rare but serious risks like pancreatitis make close monitoring and careful meal selections important. Lots of folks discover that nutritional adjustments can assist with side effect management and bolster general health while on retatrutide.
For Nausea
-
Consume five or six small meals a day instead of three large ones.
-
When symptoms flare, stick with bland foods like rice, toast, or bananas.
-
Sip fluids slowly throughout the day to stay hydrated.
-
Avoid foods with strong smells or heavy spices.
-
Keep snacks like crackers close by for quick relief.
Nausea is the most common side effect during the first few weeks and after dose increases, so eating smaller, more frequent meals is a feasible way to keep nutrition on target without overloading the stomach. Ginger, in tea or tiny candies, is soothing.
Herbal teas such as peppermint or chamomile soothe the stomach, providing mild relief. Avoid eating rich, greasy meals, which can exacerbate nausea and impede recovery. Everyone is different, so it’s helpful to keep track of which foods soothe and irritate.
For Constipation
A fiber-rich diet comprising whole grains, legumes, fruits, and vegetables is critical for maintaining regularity, particularly because constipation impacts approximately one-third of users at increased doses. Drink a minimum of 1.5 to 2 liters of water a day to assist fiber in doing its job.
Adding yogurts with live cultures or fermented foods like kimchi can support your gut, as probiotics aid digestion. Even regular walks, stretching, or gentle exercise can get things flowing. Eating slowly and chewing food well assists the gut in nutrient absorption and keeps meals comfortable.
For Fullness
-
Prepare meals in advance that balance protein, fiber, and healthy fats.
-
Avoid grazing or snacking between meals.
-
Choose whole foods instead of processed snacks to combat hunger.
Well-rounded meals with lean proteins, vegetables, and whole grains ensure you don’t feel the need to snack while still respecting the fullness that retatrutide can induce. Fats from nuts, seeds, avocado, or olive oil provide a sustained feeling of fullness and keep energy stable.
Mindful eating, which involves listening to hunger and fullness cues, can stop overeating in its tracks and keep individuals scaling back portions when necessary. Everyone’s reaction is different; some discover they require fewer servings, while others have to change meal times.
Sample Meal Framework
A sample meal plan for retatrutide users should promote wellness and be sustainable. Balanced nutrition, variety, and flexibility matter most as the medication may alter appetite and digestion. Eat meals consisting of protein, healthy fats, fiber, and slow-digesting carbohydrates. Balance, portion control, and hydration are important, and planning ahead can simplify your day.
Breakfast Ideas
Protein at breakfast helps fuel your day with consistent energy, particularly when appetite tends to be suppressed following the morning rise. Easy options are hard boiled eggs, plain Greek yogurt or tofu scramble. Pair with whole grain toast, oats or quinoa for both fiber and slow release carbs.
Top with berries, apple slices or a banana for extra vitamins and minerals. A hearty breakfast will stabilize hunger and keep you from eating too much later in the day. Hitting a balance of macros early helps steady blood sugar.
For something fast, think overnight oats with chia and sliced fruit or a smoothie with plant milk, spinach, nut butter, and frozen berries.
Lunch Ideas
Lunch is a great opportunity to squeeze in lean proteins, healthy fats, and plenty of veggies. Grilled chicken or baked salmon, chickpeas or lentils work well. Construct salads using mixed greens, tomatoes, avocado, cucumber, and a sprinkling of nuts.
Dress with olive oil or lemon. Whole grain wraps or brown rice bowls with roasted veggies and beans are both satisfying and simple to prepare. Meal prep—cook proteins or grains in bulk and store in containers, which is a time saver.
What a good serving size is, so measure portions or use smaller plates. When I eat mindfully and tune into my hunger and fullness cues, lunch is more satisfying. Dinner leftovers can be wrapped or tossed in a salad for a whole new meal, reducing waste and hassle.
Dinner Ideas
Dinner should be hearty in nutrients, but not too filling as appetite tends to wane in the evening. How about grilled fish with steamed broccoli and sweet potato or stir-fried tofu with mixed vegetables and brown rice?
Splash the plate with carrot, spinach, or red pepper to add more nutrients and color. Go for a light meal to ease digestion before sleeping. No heavy, greasy, or sugary meals late at night.
I love the family-style meals with shared dishes because it encourages healthy options and can be more fun for everyone to eat.
Snack Ideas
|
Snack |
Key Nutrients |
Benefits |
|---|---|---|
|
Apple + almond butter |
Fibre, healthy fat |
Satisfies and curbs hunger |
|
Greek yogurt & berries |
Protein, vitamins |
Supports muscle & gut health |
|
Carrot sticks & hummus |
Fibre, protein |
Crunchy, filling, portable |
|
Mixed nuts (30g) |
Healthy fat, protein |
Easy, portion-controlled energy |
Snacks should be managed to prevent overindulgence. Fruit, nuts, and yogurt provide extended satiation. Conscious snacking, such as eating screen-free, stops you from nibbling due to habit rather than hunger.
Water is important, as some medications can blunt thirst.
Beyond The Plate
Gazing past the fork, health outcomes with retatrutide are about more than what’s on the plate. Lifestyle, mental well-being, and social connections all form how effective this medicine is and how sustainable forward movement becomes. Diet is only one part.
Other things, like meal timing, stress, and community, contribute as well.
The Gut Microbiome
Gut health connects intimately with everything from digestion to nutrient breakdown to weight management. A healthy gut microbiome, a mix of bacteria, fungi, and viruses, aids in digesting fiber, keeping inflammation down, and promoting balanced metabolism.
Tiny gut bacteria shifts can alter energy expenditure and blood glucose management. What you eat counts. Fiber rich legumes, fruits, and whole grain diets provide food for good bacteria.
Fermented foods boost gut health, like yogurt, kefir, kimchi, and sauerkraut. Too many refined carbs can throw things off, sometimes causing bloating or discomfort. Keeping track of what you eat and any symptoms can assist in determining which foods benefit or irritate your gut.
For most, targeting 21 to 30 grams of fiber per day goes a long way, providing digestive and weight management upsides. Aside from the plate, a balanced gut microbiome enables weight loss and makes it easier to combat side effects such as constipation, which can impact up to 33% of those on some medications.
The Mental Aspect
It’s not just about eating. Beliefs, emotions, and behaviors influence decisions. Stress, boredom, or sadness can drive us to eat more or seek out less nutritious options.
Mindfulness, paying attention to hunger, taste, and fullness, can help you build a better relationship with food and body image. Realistic, not extreme, goals help keep motivation high and setbacks in check.
Eating frequent small meals can alleviate nausea or heartburn, allowing the body to digest food more efficiently. Prioritizing protein first and then taking a pause tames appetite. This is a great strategy given retatrutide can decrease appetite.
Support is queen. Talking with a counselor or dietitian or joining a group can provide helpful tools and encouragement to get through the rough patches. Tracking food and symptoms over time can help you determine patterns, like whether refined carbs cause unwelcome reactions or if certain habits lend you better energy.
Exercise counts as well. Even 20 minutes a couple of times a week can sustain mood, metabolism, and blood sugar. Exercise and stress relief with easy habits such as deep breathing or mini walks keep body and mind in sync.
Conclusion
To optimize retatrutide, consume balanced meals comprising whole foods. Reach for lean meat, beans, whole grains, and plenty of fresh fruit and veggies. Hydrate yourself sufficiently. Keep your meals simple, with bright colors and varied textures, so eating is pleasurable and not a chore. Pay attention to how your body feels following meals. Tinker with your diet if you experience stomach issues or fatigue. Attempt to be a little active every day, even if it’s just a stroll. Consult your physician or dietician if you have questions or want to make large adjustments. For additional pointers or actual meal suggestions, visit in-person groups or reliable online forums. Tiny tweaks accumulate.
Frequently Asked Questions
What foods should I eat while taking Retatrutide?
Pay attention to balanced meals with vegetables, whole grains, lean protein, and healthy fats. Minimize processed foods and sugar-sweetened beverages. This complements Retatrutide’s impact and encourages holistic wellness.
Are there foods I should avoid on Retatrutide?
Yes, stay away from fried foods and sugars. These can exacerbate side effects such as nausea or delay weight loss outcomes. It is best to eat light, healthy meals.
How should I time my meals with Retatrutide?
Have small meals throughout the day. This prevents you from getting hungry and stabilizes your energy. Skip big or heavy meals, which can increase side effects.
Can I drink alcohol while using Retatrutide?
Try to cut back on or avoid alcohol. Alcohol may worsen stomach upset and can influence blood sugar levels. As always, consult your doctor for personalized advice.
What can I do if I feel nauseous on Retatrutide?
Go for bland low-fat foods such as crackers, rice, or bananas. Take small sips of water. Try eating smaller, more frequent meals, which can minimize nausea.
Do I need supplements with Retatrutide?
Supplements are rarely required if you consume a nutritious diet. If you have specific deficiencies, talk to your provider before supplementing.
Can Retatrutide replace healthy eating?
No, Retatrutide loves a healthy diet. Healthy nutrition will aid in your weight loss and in your overall health. Take both for maximum effect.