Key Takeaways
-
Start lymphatic massage when your surgeon gives the green light, typically within the first week. Guide yourself through a gradual, structured schedule as you recover.
-
Frequent lymphatic massage decreases swelling, reduces the risk of fibrosis, and helps you feel more comfortable during your recovery from a Brazilian butt lift.
-
Make sure to always use a licensed therapist who specializes in post-operative care.
-
Timely intervention is key. Starting too early or too late could impede healing or extend swelling, so heed professional advice closely.
-
Work with your therapist to customize your massage schedule, modifying frequency and methodology according to your surgery and your own healing progression.
-
Emotional well-being is important for recovery. Use massage sessions to include relaxation techniques and reach out for support when you need it.
Most surgeons recommend you begin lymphatic massage approximately 24 to 48 hours after a BBL surgery, once your doctor says it is safe. It helps reduce swelling and fluid build-up and may encourage faster healing.
All cases are unique, so always consult with your care team prior to scheduling a session. The following sections discuss why timing is important, what to anticipate, and how to locate expert assistance.
Optimal Timing
Lymphatic massage is essential to BBL patients’ post-surgical recovery. The ideal time to begin is once your surgeon gives the okay, typically about 5 to 7 days post-surgery. This window lets the incisions start healing, which reduces the risk of complications. Most surgeons recommend waiting around a week, but the timing depends on your body and how your wounds are healing.
Below is a simple numbered list outlining a typical schedule for lymphatic massage after a BBL procedure:
-
Begin with mild lymphatic drainage 5 to 7 days post-operation, once your doctor gives the OK.
-
In week 1, daily sessions keep the extreme swelling and fluid accumulation under control.
-
From weeks two to six, frequency reduces to 2 to 3 times per week as healing continues.
-
Once every six weeks, weekly, or biweekly maintenance sessions to maintain recovery and tissue health.
1. Immediate Post-Op
Mild lymphatic drainage can be initiated within the first few days post-surgery, only with your surgeon and licensed therapist’s direction. The goal is efficient removal of surplus fluid from operative sites, particularly in the presence of incisional drainage. During this phase, swelling can be at its worst, and massage can help alleviate pain and fluid retention.
Untrained hands should not do the massage because it can put pressure on tissue that is still healing. Listen for pain, redness or increased swelling and discontinue if these appear.
2. The First Week
For most patients, daily lymphatic massages are best in the initial week! The stroke should always be superficial, never deep or vigorous. Even minor fluctuations in pressure can be painful or stall recovery.
I recommend maintaining an open dialogue with your massage therapist to monitor pain and progress. Always heed specific instructions from your surgeon on how frequently to massage and where, because some patients heal faster than others.
3. Weeks Two to Six
While swelling goes down and incisions heal, students typically receive 2 to 3 massages a week. This consistent timing encourages lymphatic drainage and minimizes fibrosis. Light exercise, such as walking, can facilitate lymphatic flow.
Inspect the incision sites prior to each session, and if there is any redness or irritation, inform your therapist and modify the technique. Good hydration, balanced nutrition, and sleep all contribute to helping tissue repair during this period.
4. Long-Term Care
After six weeks, most patients transition to weekly or biweekly lymphatic massages. This aids in preserving results and handling any residual swelling. Continuous massage can help loosen scar tissue and avoid irregular healing.
Self-care counts, as well. Hydrating and being active can help your lymphatic system in between appointments. Be on the lookout for any new lumps, bumps, or changes and check in with your therapist if you notice anything that feels ‘off’.
Recovery Benefits
Lymphatic massage after BBL has specific benefits that help facilitate a healthy recovery. This therapy is well known for its gentle, rhythmic strokes that aid in flushing out excess fluid, relieving swelling and supporting tissue repair. Regular lymphatic drainage treatments can help patients experience less discomfort, prevent the formation of hard scars, and improve the aesthetic appearance of the surgical site.
Below are the main recovery benefits:
-
Diminishes swelling and excessive fluid retention for a speedy recovery.
-
Minimizes the risk of fibrosis and hardened scar tissue.
-
Supports healthy skin texture and smoother contour.
-
Lowers discomfort, pain, and post-surgical soreness.
-
Helps prevent complications like seromas and hematomas.
-
Improves sleep, mood, and overall sense of well-being.
-
Boosts metabolism and encourages better nutrient flow to tissues.
-
Leaves many people feeling lighter and “refreshed” after sessions.
Reduce Swelling
Lymphatic drainage massage attacks swelling that’s common post-BBL. The body has the tendency to retain fluid following surgery, which impedes healing. With slow, gentle strokes, it can direct this additional fluid back into the lymphatic system.
Over time, this helps reduce inflammation, accelerates recovery, and prevents the area from becoming too swollen. Most people thrive on 2 to 3 sessions per week for the first month. This simple consistency helps keep swelling in check.
Light self-massage, when conducted properly, can assist between visits. As always, check with a qualified therapist or your surgeon before attempting this at home! Monitoring the changes in swelling on a weekly basis can help customize the number and type of sessions required.
For some, swelling reduces rapidly; for others, additional time and assistance is needed.
Minimize Fibrosis
Frequent lymphatic massage prevents the formation of hard, dense tissue known as fibrosis. When excess fluid remains in one place for a prolonged period, the body might respond by developing hardened regions. These can cause the skin to feel taut or appear patchy.
Careful scar tissue massage paired with compression garments can keep tissues soft and pliable. Be alert to the early signs of fibrosis, such as lumps, hardness or thickening under the skin. Report these changes to your therapist.
Early detection catches problems when they are easiest to fix.
Enhance Results
Lymphatic massage benefits the final appearance of a BBL by contouring the skin. Good lymph flow ensures that cells receive the necessary nutrients for robust healing. Together with good nutrition and hydration, massage helps to maintain the new tissue healthy and supple.
Share with your therapist any changes you notice. Others experience more defined contours and firmer skin after just a couple of treatments.
Improve Comfort
Light massage is great for relieving soreness and pain. This is most particularly the case post BBL when comfort can be elusive. Soft strokes provide comfort by circulating fluid, reducing lactic acid and soothing the patient.
Discussing pain or stress openly with your therapist allows him or her to tailor each session to your needs. Deep breathing during massage can reduce stress and increase relaxation.
Potential Risks
Post-operative lymphatic massage after a BBL can reduce swelling, relieve pain, and promote healing. The process has risks if not timed or executed properly. Not everyone is going to require lymphatic massage. Some people do fine with compression garments alone, and meticulous surgical technique can reduce the need for additional therapy.
Make sure to discuss this with your surgeon and therapist to figure out what’s best for your situation since the benefits and risks can vary depending on the type of surgery and your health.
Do’s and Don’ts of Lymphatic Massage:
-
Do follow your surgeon’s instructions and post-op plan.
-
Do use compression garments and foam pads as advised.
-
Do monitor your swelling and overall comfort.
-
Do choose a therapist with post-op training.
-
Don’t start massage too soon or too late.
-
Don’t ignore pain or unusual symptoms during sessions.
-
Don’t rely on massage alone—combine with other recovery steps.
-
Don’t skip regular follow-ups with your doctor.
Starting Too Early
Initiating lymphatic massage prior to receiving the green light from your surgeon can exacerbate swelling and pain. Tissues are vulnerable immediately post-op, and too much pressure can harm healing fat cells or skin, resulting in sub-optimal outcomes or extended downtime.
The majority of surgeons suggest waiting 7 to 14 days, but this can vary. Pay attention to your body. If you experience sharp pain, new bruises, or additional swelling, cease and consult with your medical team. Massage may work early, but it is more critical to allow your body time to settle.
Starting Too Late
Waiting too long to start lymphatic massage can allow swelling to hang around and prolong your recovery. Persistent swelling can increase the risk of scar tissue forming in undesirable places. Early treatment assists lymph flow and drains fluid from swollen regions.
Still, massage isn’t necessary for everyone. Other research finds no significant benefit beyond compression gear. If you procrastinate massage, consult with your therapist regarding your schedule and requirements, and be aware of symptoms of fluid accumulation or seromas.
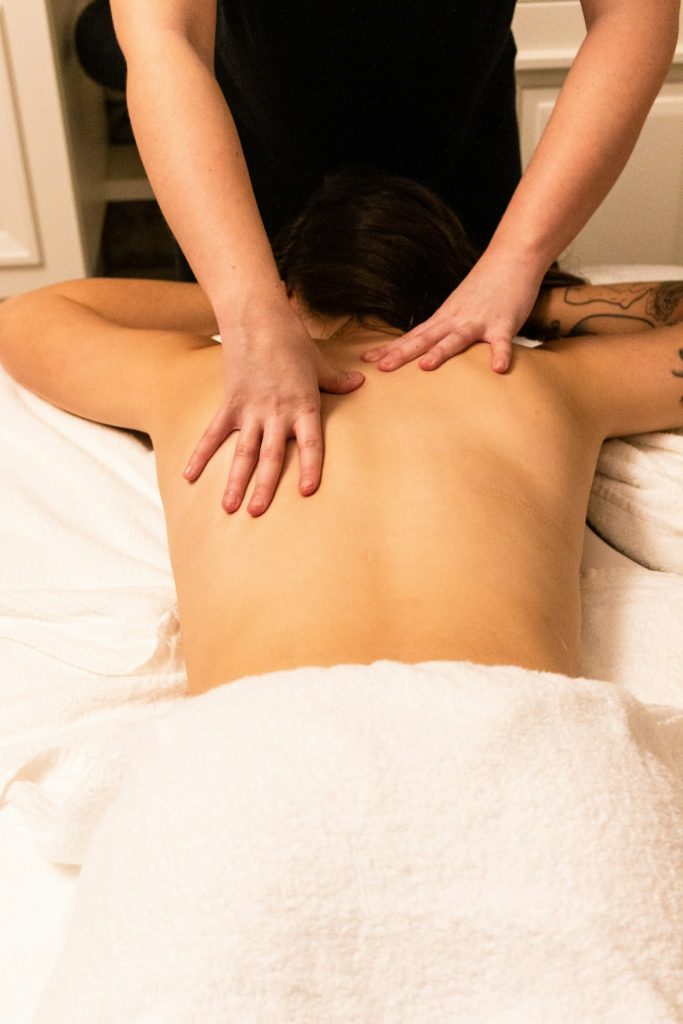
Take an active role in your own recovery, but temper it with patience and guidance from your care team.
Improper Technique
Applying the incorrect type of massage can actually exacerbate the symptoms. Bad technique can damage sensitive tissue, rupture scars, or drive fluid where it doesn’t belong. Select a therapist with actual post-op lymphatic drainage training.
It helps to know what being good looks and feels like, so you can provide feedback. Let your therapist know if any stroke aches or feels ‘wrong’. Not all massage types are appropriate for all surgery, so verify with your physician.
Others experience just a quick reprieve and some don’t need massage at all if their edema is light or their surgeon is exceptional.
Finding Your Therapist
Post-BBL surgery, the proper lymphatic massage can accelerate recovery and reduce the risk of swelling or lumps. Selecting a therapist for this work requires more than a quick hunt. It’s about trust and skill and how comfortable you feel with them. A simple checklist keeps the process on track.
First, make sure your therapist has recent training and experience in lymphatic drainage massage, not general massage. Seek demonstrable work with post-surgical clients, particularly BBL clients, and request their skill certificates. Next, look at their specialties. Some therapists work primarily with cosmetic surgery recovery, while others may cover more general areas. Find one who understands the unique care BBL patients require.
Ask your surgeon or recovery team for names of therapists they trust. Most clinics partner with massage pros that are familiar with how and when post-BBL care should be administered. This can help you bypass unqualified options. If you need additional possibilities, ask friends, family, or even your general practitioner for suggestions.
Others like to browse online directories, reviews, or their health insurance network if lymphatic massage is included. Both routes have their advantages. Referrals generally imply a higher level of trust, whereas online searches demonstrate a greater breadth of options. Don’t feel weird about sampling a few before you find the right fit. Your comfort is important, and studies indicate that the relationship between you and your surgeon can influence your post-surgery outcomes.
Arrange a meeting or phone call before you commit to sessions. This is your opportunity to discuss your recovery plan, inquire about their experience with BBL patients, and confirm you are aligned. Inform them of your surgery date, any apprehensions, and expectations of the massages.
Some people want a therapist who is the same culture or age as them. Others just want the right skill sets. Be candid about what makes you feel secure and understood in your healing. If you feel a disconnect or do not feel good about it, it is okay to continue the search for a better fit.
The initial moments in discovering your therapist can be hard, particularly if you’re a newcomer to post-surgery care or this type of massage. Going slow, asking the right questions, and gut checking can ease the process.
Personalizing Your Plan
Your individualized lymphatic massage plan is influenced by your specific health background, your surgical specifics, and your recovery process. In collaboration with your therapist and surgeon, you can schedule out a plan that best suits you and facilitates safe, gradual recovery. Changes are the norm during healing. We continue to check in and adjust frequency, modalities, and timing.
Your Health
Taking stock of your general health helps steer your massage plan from the beginning. Chronic conditions like diabetes, heart disease, or autoimmune disorders might require specific modifications. Discuss any health history or medications with your therapist prior to starting treatment. This prevents it from getting complicated and keeps your plan secure.
Listen to your body during recovery. Pay attention to indicators like inflammation, bruising, or pain and utilize these as a guide for when to initiate or suspend massage. If you have a fever, abnormal redness, or stabbing pain, then stop sessions and contact your medical team.
Wellness habits such as hydration, light exercise, and proper nutrition can complement your results. These little daily decisions keep lymph moving and enhance the efficacy of every massage.
Surgical Complexity
The nature and degree of surgery influence your schedule. Less invasive surgeries may require just a few sessions, while intricate procedures such as BBL, full abdominoplasty or Lipo 360 frequently demand six to ten or more. As always, talk with your surgeon to find out how your particular surgery modifies your plan.
With an emphasis on treated regions and scaling techniques to the extent of tissue damage. For instance, high-volume liposuction may require more gradual and delicate passes initially. Smaller fat grafts could be eligible for typical methods earlier.
Personalizing your plan requires patience with the process. Surgeons recommend that the first massage be initiated sometime within the first week, only if healing is progressing appropriately. Too much, too soon can stall recovery or cause complications.
Massage sessions last 30 to 60 minutes and might begin at 2 to 3 times per week, evening out as swelling subsides.
Your Body’s Signals
|
Body Signal |
What It Means |
Massage Adjustment |
|---|---|---|
|
Mild swelling |
Normal post-op |
Continue as planned |
|
Redness/warmth |
Possible infection |
Pause, consult doctor |
|
Sharp pain |
Healing concern |
Reduce pressure, notify team |
|
Less swelling |
Progressing well |
Gradually decrease sessions |
|
Stiffness |
Scar tissue forming |
Add gentle stretching |
Session frequency and timing should align with your core body response. Some patients receive maintenance sessions for two to three months, particularly if swelling lingers or fibrosis is a risk.
Constantly provide feedback to your therapist, particularly if you feel uncomfortable or if symptoms shift. Trust your gut—if it feels off, tweak your plan.
The Emotional Component
Healing from surgery, such as a BBL, is not simply physical. A lot of people experience the emotional component as much as the physical healing. Post-surgery, individuals can experience anxiety, tension, or even depression. The physical changes and the downtime post-surgery can elicit all sorts of emotions. For a lot of people, this is a hard season and solid support counts.
Lymphatic drainage massage can assist here, not just for the swelling but for how you feel internally. The soft touch and slow motion of these massages can calm. A lot of folks report feeling less stressed and more relaxed post-session. It’s not all in their heads—research indicates that lymphatic massage reduces stress and a few even observe reduced symptoms of depression or anxiety after these massages.
Employing relaxation techniques during massage can assist. Deep breathing, soft music, or a calm room can help you relax as you receive your massage. It’s these little things that make the difference. You may notice your mind begins to decelerate and anxiety dissipates slightly.
The massage assists your body in eliminating waste and swelling. Simultaneously, it provides a respite for your brain. They report that they walk out of their appointment feeling lighter—not just in their body but in their mood. This calm can persist for hours or even days, providing you with an essential uplift throughout your recuperation.
It’s good to discuss with your therapist your emotions. A good therapist understands that recuperation isn’t only physical. If you’re concerned or curious, inform them. This can transform the rub into a sanctuary where you can bare your thoughts.
It will build trust and calm your mind. Others report that they feel more prepared to take on the day following a strong talk and massage. It’s not simply the hands-on work but having someone who will listen to you and care.
Recovering from surgery is a slow journey. It can be an opportunity to decelerate and take care of yourself. For most, this is an opportunity to understand their own needs and what makes them feel better.
Prioritizing massage and self-care can make you feel stronger, inside and out. You might become more confident and prepared to return to normal life. Lymphatic massage is one of those ways, supporting your body and your mind as you heal.
Conclusion
When to kick off lymphatic massage after BBL Most surgeons recommend starting during the first week as soon as your body feels up to it and your doc gives the green light. Lymphatic drainage massage is a gentle, rhythmical massage that stimulates movement of lymph fluids around the body. Selecting a certified therapist with actual post-op experience matters. Just remember that everyone heals differently, so follow a routine that aligns with your body and your needs. Keeping in tune with how you feel can help you manage stress and improve your spirits as you recover. For specifics or advice, consult your surgeon or experienced massage therapist. Ready to move forward? Get answers and schedule your care with the right pros.
Frequently Asked Questions
When can I start lymphatic massage after BBL surgery?
Most surgeons suggest beginning lymphatic massage five to seven days post BBL surgery. Always get clearance from your doctor before starting any massage.
Why is lymphatic massage important after a BBL?
Lymphatic massage reduces swelling, improves circulation, and prevents fluid build-up. This helps accelerate healing and enhances your results.
Can lymphatic massage reduce pain after BBL surgery?
Yes, soft lymphatic massage can relieve pain, alleviate tightness and make you feel more comfortable during healing.
Are there risks with lymphatic massage too soon after BBL?
Beginning massage too soon or too hard can damage healing tissues, elevate infection risk, or lead to complications. Always listen to your surgeon.
How do I find a qualified lymphatic massage therapist?
Select a therapist that has experience in working with post-surgical patients. Ideally, choose one with specialized training in lymphatic drainage for cosmetic surgery. Request credentials and reviews.
How many lymphatic massages will I need after BBL?
Many patients require multiple sessions, sometimes two to three times per week, for the initial few weeks. Your doctor will suggest a schedule depending on your individual needs.
Can lymphatic massage affect my emotional recovery after BBL?
Yes, massage can induce relaxation, ease your stress, and nurture your emotional health throughout your recovery process.





